Marc Salcedo
Our Frontline Healthcare Heroes
BS '14, Nursing
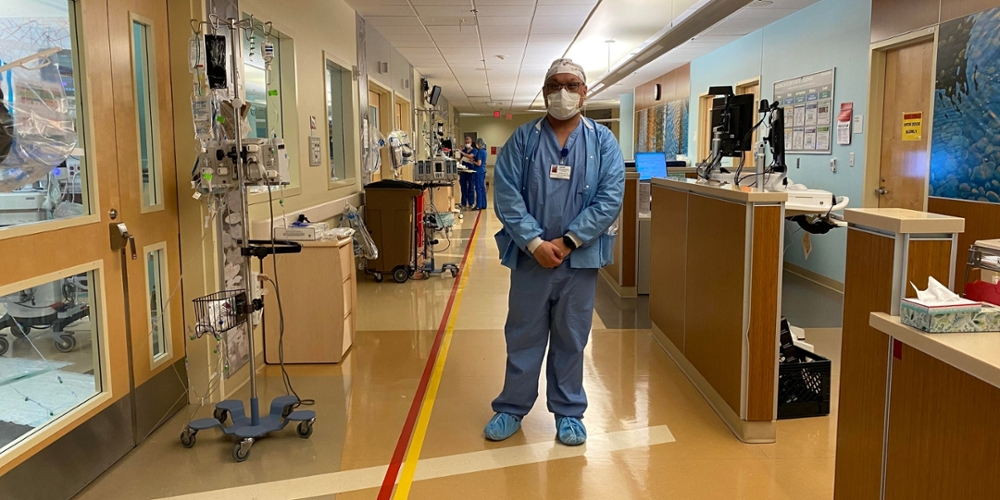
Marc Salcedo BSN, RN, CCRN (BS '14, Nursing) works for Kaiser Permanente in the Intensive Care Unit. As a nurse in the frontlines, he is taking care of patients that have or could have COVID-19.
The hardest thing about it is first getting over the fear of possibly contracting the disease or spreading it to family and friends. Though Marc likes to keep things positive, "Working in the ICU can be emotionally taxing, but also extremely rewarding. You are the healing hand when patients are usually at their worst. While it’s tough all around for everyone, I have felt the love and support of the community. All of this support really gives us a boost in our morale, and we are all forever grateful for the support," said Marc.
Q&A with Marc
Why did you decide to attend Cal State East Bay?
As a Hayward resident, Cal State East Bay was well known to me. In my childhood, I would always see Warren Hall towering above the hills and wondered how it would be like to attend. I wasn’t sure of what career path to take but was interested Pre-Law and Pre-Nursing, both of which were offered by East Bay. When I got my acceptance letter and saw the financial aid package, I knew that the university was a perfect fit for me. East Bay provided me an education without putting me into enormous amounts of college debt. Plus my childhood dream of being able to go to school with the big tower has come true.
How has your education at East Bay helped you with your endeavors? What are some of your goals?
My education at East Bay has given me a well-rounded education. Not only did I get a good foundation in my degree of Nursing, I was able to explore other areas and received minors in the Health Sciences and Chinese Language & Cultural Studies. My studies in Health Studies has given me a better understanding of our healthcare system. I speak Mandarin Chinese for my patients that primarily comprehend it. I also have an awareness on Chinese cultural beliefs and attitudes regarding health. I feel all of these help in how I provide patient care. My short term goal is to go through my job’s clinical ladder program and be designated as a Staff Nurse III. My long term goal is to get a graduate degree in Nursing, focusing to be either a Nurse Practitioner or Nurse Anesthetist.
Did you face any challenges at Cal State East Bay? If so, how did you handle them?
I felt the entire Nursing program was a challenge in itself. When I went to East Bay it was under the Quarter System. In the second year, we had rotations (2 in a quarter, 5 weeks each) on top of having regular nursing classes. A rotation in the beginning of the quarter would have a final in the middle of the quarter, alongside your midterms. Plus the tests sometimes would have multiple choice, select all the above questions that require you to pick the most correct answer. In the summer before the second year, my mother had multiple surgeries which made it even more difficult for me as I had to juggle taking care of her and studying for nursing classes. I simply took things one at a time. I learned to find out what my resources were back then and reached out to people when I felt overwhelmed and needed help. I am extremely grateful for the support my family and friends have given during that time, including faculty. Everyone in nursing school supported one another as we knew we were all in the same boat, the same journey. I remember those long group study hours even after we graduated when we were studying for the nurse licensure exam.
Tell us about your career journey and your current job.
My career has taken me from East to West. When I graduated, new-graduate nursing jobs were competitive and hard to come by in California. After a year of applying, I decided to move to the Washington DC area where some of my family lived and was able to secure a job at a Level 1 trauma hospital in Northern Virginia for their ICU step-down unit. Even though my experience in the DC area was wonderful, I was still sorely homesick. Although not exactly in the Bay Area, I took an ICU Step-down position in Modesto and slowly made my way back. During this time, I realized that I wanted to work in the Intensive Care Unit. When the opportunity came, I took a position in the Bay Area where I worked in a hospital that provided training to the ICU.
Currently, I work for Kaiser Permanente in an Intensive Care Unit. We take care of patients who need closer monitoring and require more support, such as needing the use of the ventilator or medications that require more monitoring. We provide complex but compassionate care to our patients and their family. We are advocates for our patients and collaborate with the health care team. I also have been trained into the Rapid Response Team role, where you become a resource for fellow nurses in the hospital when they are concerned their patients are becoming unstable and respond to inpatient emergencies known as a Code Blue. I am involved in my unit by participating in committees, dedicated to improving patient care. After long hours of studying and passing the test, I eventually became a certified Critical Care Nurse (CCRN).
Working in the ICU can be emotionally taxing, but also extremely rewarding. You are the healing hand when patients are usually at their worst. It makes you feel good when you are able to make a difference in a person’s life. It is impossible to work in this career without the support of my coworkers: nurses, respiratory therapists, doctors, pharmacists, phlebotomists, and many more working as one to provide the best care to our patients.
What has been the biggest challenge you are facing while combatting the coronavirus?
As a nurse in the frontlines, I am taking care of patients that have or possibly have the coronavirus or properly known as COVID-19. The hardest thing about it is first getting over the fear of possibly contracting the disease. What makes it even worse is the possibility of somehow spreading it to our family and friends. I am fortunate that currently, my mother is not living with me at home as my biggest fear is that I expose her to the disease. She has multiple ailments that put her at a higher risk of getting severe symptoms. But I have seen some of my coworkers having to move out and/or even avoid personally interacting with their loved ones out of fear of spreading it to them. Many of us have new time-consuming routines for work. I usually change into a different pair of scrubs while at work and change into new ones before going home. At home, I have a disinfection station where I clean all that I have to bring in from work and have a separate linen basket lined with a trash bag for anything I have worn that day. Afterward, I take a long hot shower to make sure I wash off anything I might have been exposed to. At work, we change our gloves often to prevent self-contamination as we take each Protective Personal Equipment (PPE) off and have to sanitize our hands in between changing gloves. All the repetitive washing and sanitizing have taken a toll on my skin, drying it out.
Given the situation, visitation to the hospital has been extremely limited. We have been trying our best to provide support for our patients so they don’t feel they are alone and update their families as much as possible. COVID-19 is no joke, I have patients that end up being on ventilators requiring high amounts of oxygen, and some ultimately pass away. Thus it is extremely important for all of us to be extremely careful and vigilant, following the latest guidelines.
While it’s tough all around for everyone, I have felt the love and support of the community. It is known that there’s a short supply of PPE and yet we have amazing people donating them to us. I would like to give a shout out specifically to my coworker Michelle Diaz and her team at Make Me PPE Bay Area for their donations. I would like to thank the California Nurses Association for vigorously advocating for a safe working environment. I can see how the management team at work are trying to provide a safe working environment, despite having to ration out PPE. We also had generous donors providing us with meals at work. We have received lots of cards and signs showing appreciation for what we do. All of this support really gives us a boost in our morale and we are all forever grateful for the support.
What is your fondest memory at CSUEB?
My fondest memory was the people, everyone was so nice and accommodating. I remembered being a part of the Asian American Pacific Island Serving Institution Program called SSOS. I met and worked with a wonderful group of people, discussing our cultural identities and social issues facing our community. When I worked for SSOS, part of my job was to encourage and help fellow students talk about their personal stories and share them. I cherish these long intimate chats inside the trailer. SSOS allowed me to attend conferences and even provided opportunities for public speaking. I felt all that I learned from this program has helped me in my current career. I want to give a shout out to Dr. Meiling Wu and Dr. Kim Geron, as they were advocates for SSOS. I am grateful for the opportunity they gave me and the experiences I was able to have because of the program.
If you could share one piece of advice with Pioneer students, what would that be?
I would say the best advice I can give students is to be open to going out of their comfort zones. After I graduated from nursing school, I always thought that I would work in a Medical/Surgical or Telemetry unit. Never did I dream to work in Critical Care. If I didn’t move to the East Coast and eventually Modesto, I would never have had the confidence and drive to pursue working in the ICU. When I was applying for my first nursing job, the Intermediate Care (step-down ICU) unit in Northern Virginia offered me a position. Despite not feeling confident enough, I took the challenge and accepted the job. I have met many people along the way that inspired, supported, and pushed me to be the best nurse I can be. There are different sets of people and cultures with differing views in Northern Virginia/Washington DC and Modesto. Moving to these places broadened my understanding of the world. When I first moved to the East Coast, my cousin has told me that I should pursue to become a Nurse Anesthetist. At that point, I had always dismissed him since I didn’t have confidence, but in the end, he can have the last laugh as I am now considering it. Moving away from home can be frightening, but if you are lucky enough to be surrounded by the right people, then it would be the most rewarding experience you can have.